
the comprehensive clinician’s guide to cognitive behavioral therapy
CBT skillfully alters negative thought patterns, profoundly impacting mood and behavior, offering treatment for anxiety, depression, and addiction – a versatile approach.
Adapting irrational thoughts, the core of CBT, has widely permeated mainstream understanding, influencing how we approach mental wellbeing and emotional regulation.
Trauma-Focused CBT (TF-CBT) provides a safe therapeutic space for children navigating traumatic experiences, fostering resilience and healthy coping mechanisms.

Cognitive Processing Therapy (CPT) effectively addresses PTSD by challenging and reshaping perspectives on traumatic events, promoting emotional healing and recovery.
Behavioral therapy, encompassing various techniques, posits that learned behaviors can be modified, offering pathways to overcome mental health challenges effectively.
What is CBT?
Cognitive Behavioral Therapy (CBT) is a collaborative, goal-oriented psychotherapy rooted in the conviction that our thoughts, feelings, and behaviors are interconnected. It’s not simply about feeling better; it’s about learning to feel better through practical skills and strategies. CBT operates on the principle that psychological distress often stems from unhelpful or inaccurate thinking patterns.
Essentially, CBT helps individuals identify and challenge these negative thought patterns, replacing them with more balanced and realistic ones. This isn’t about positive thinking, but rather about accurate thinking. Simultaneously, CBT focuses on modifying behaviors that contribute to emotional distress. It’s a highly structured approach, often involving homework assignments and active participation from the client.
The therapy isn’t a lengthy exploration of the past, though past experiences may be relevant. Instead, it’s primarily focused on present problems and developing coping mechanisms for the future. CBT is evidence-based, meaning its effectiveness has been demonstrated through rigorous scientific research, making it a widely respected and utilized therapeutic modality.

The Core Principles of CBT
Central to CBT is the understanding that psychological problems are, in part, maintained by cognitive distortions – inaccurate or unhelpful ways of interpreting experiences. These distortions influence our emotional responses and subsequent behaviors, creating a vicious cycle. A key principle is the belief that individuals are not victims of their circumstances, but rather active participants in shaping their own experiences.
Another foundational tenet is the importance of the therapeutic relationship. CBT is collaborative, with the therapist acting as a guide and the client as an active learner. Emphasis is placed on identifying specific, measurable, achievable, relevant, and time-bound (SMART) goals.
Furthermore, CBT is empirically driven, meaning techniques are based on scientific evidence and regularly evaluated for effectiveness. It’s a present-focused approach, prioritizing solutions to current problems over extensive exploration of the past. Finally, CBT emphasizes self-empowerment, equipping clients with skills to become their own therapists.
Historical Development of CBT
The roots of CBT trace back to the early 20th century, with influences from behavioral and cognitive psychology. Ivan Pavlov’s classical conditioning and B.F. Skinner’s operant conditioning laid the groundwork for understanding how behaviors are learned and modified. However, it was Aaron Beck’s work in the 1960s that truly sparked the cognitive revolution.
Beck, while treating depressed patients, noticed the prevalence of negative automatic thoughts and cognitive distortions. Simultaneously, Albert Ellis developed Rational Emotive Behavior Therapy (REBT), emphasizing the role of irrational beliefs in emotional distress. These parallel developments converged to form the foundation of CBT.
Throughout the 1970s and 80s, CBT gained prominence as research demonstrated its effectiveness in treating various disorders. Modifications and specializations emerged, like Trauma-Focused CBT, expanding its applications. Today, CBT continues to evolve, integrating new findings and technologies, remaining a leading psychotherapeutic approach.
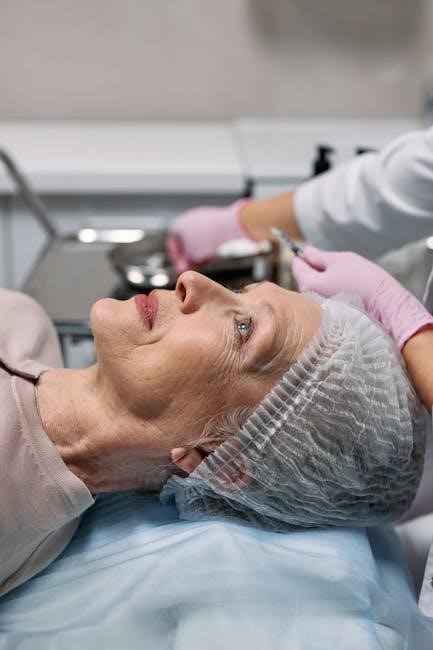
Key CBT Techniques
CBT employs diverse techniques—cognitive restructuring, behavioral activation, and exposure therapy—tailored to individual needs, offering a flexible and effective therapeutic toolkit.
Cognitive Restructuring
Cognitive restructuring, a cornerstone of CBT, centers on identifying and modifying negative or unhelpful thought patterns that contribute to emotional distress. This process isn’t about simply “thinking positive,” but rather achieving a more balanced and realistic perspective.
Initially, therapists guide clients in identifying negative thought patterns – automatic thoughts that arise in response to specific situations. These thoughts are often distorted, reflecting biases or inaccuracies. Common patterns include all-or-nothing thinking, catastrophizing, and mental filtering.
Subsequently, clients learn to challenge irrational thoughts by examining the evidence for and against them. This involves questioning the validity of these thoughts and considering alternative explanations. Socratic questioning is frequently employed to facilitate this process.
Ultimately, the goal is developing alternative, balanced thoughts that are more grounded in reality and less emotionally charged. This doesn’t eliminate negative feelings entirely, but it reduces their intensity and impact, fostering greater emotional regulation and wellbeing.
Identifying Negative Thought Patterns
The initial step in cognitive restructuring involves meticulously identifying negative thought patterns – those automatic, often unconscious, beliefs that surface in response to life events. These aren’t necessarily factual, but powerfully influence our emotions and behaviors.
Clinicians assist clients in recognizing common cognitive distortions, such as ‘all-or-nothing’ thinking, where situations are viewed in extreme terms, or ‘catastrophizing,’ anticipating the worst possible outcome. ‘Mental filtering’ focuses solely on negative details, ignoring the positive.
Thought records are frequently utilized; clients document triggering situations, their associated thoughts, and resulting feelings. This externalization allows for objective examination. Recognizing these patterns is crucial, as they often operate outside of conscious awareness.
Furthermore, understanding the function of these thoughts – what purpose they serve, even if maladaptive – provides valuable insight. Identifying these patterns is the foundation for subsequent cognitive work.
Challenging Irrational Thoughts
Once negative thought patterns are identified, the next crucial phase involves challenging their validity. This isn’t about simply ‘positive thinking,’ but a rigorous examination of evidence supporting and contradicting the thought.
Clinicians guide clients to act as ‘detectives,’ questioning the thought’s basis in reality. Techniques include the ‘Socratic method’ – asking probing questions to reveal logical fallacies. Is there alternative explanations? What’s the worst that could realistically happen?
Examining the thought’s helpfulness is also key. Even if a thought is partially true, does dwelling on it improve the situation or contribute to wellbeing? Identifying cognitive distortions – like overgeneralization or personalization – aids in dismantling irrational beliefs.
The goal isn’t to eliminate negative thoughts entirely, but to reduce their power and influence, fostering a more balanced and realistic perspective.
Developing Alternative, Balanced Thoughts
After challenging irrational thoughts, the focus shifts to constructing more realistic and balanced alternatives. This isn’t about forced positivity, but crafting thoughts grounded in evidence and acknowledging nuance.
Clinicians assist clients in generating multiple perspectives, considering all available information. The aim is to move away from ‘all-or-nothing’ thinking towards a more flexible and adaptive mindset. What’s a more reasonable interpretation of the situation?
Alternative thoughts should be believable and helpful, reducing distress without dismissing genuine concerns. This process often involves reframing – viewing the situation from a different angle, highlighting strengths and resources.
Regular practice is vital. Clients are encouraged to actively replace negative thoughts with their balanced alternatives, strengthening new neural pathways and fostering lasting change.
Behavioral Activation
Behavioral activation is a core CBT technique, particularly effective in treating depression. It centers on the principle that our actions influence our feelings, rather than the other way around. Often, depression leads to withdrawal and inactivity, exacerbating negative moods.
The process involves identifying activities that once brought pleasure or a sense of accomplishment, even small ones. Clients collaboratively create a schedule, gradually reintroducing these activities into their routine.
It’s not about feeling motivated to do something; it’s about doing something, and allowing the positive feelings to follow. Clinicians help clients break down tasks into manageable steps, increasing the likelihood of success.
Monitoring mood before and after activities helps demonstrate the link between behavior and emotion, reinforcing the effectiveness of the technique and building self-efficacy.
Exposure Therapy
Exposure therapy is a powerful CBT technique used primarily for anxiety disorders, predicated on the idea that avoidance maintains fear. It involves gradually confronting feared stimuli or situations in a safe and controlled environment.
The goal isn’t to eliminate anxiety entirely, but to learn to tolerate it and reduce the associated behavioral avoidance. This process helps to extinguish the learned fear response.
Two main approaches exist: systematic desensitization and flooding. Systematic desensitization involves creating a fear hierarchy, starting with mildly anxiety-provoking situations and progressively moving to more challenging ones, coupled with relaxation techniques.
Flooding techniques, conversely, involve immediate and prolonged exposure to the most feared stimulus. While potentially more rapid, it requires careful assessment and client preparation due to its intensity.
Systematic Desensitization
Systematic desensitization, a core component of exposure therapy, meticulously addresses anxiety by pairing relaxation techniques with gradual exposure to feared stimuli. This method hinges on the principle of reciprocal inhibition – anxiety and relaxation are mutually incompatible states.
The process begins with collaboratively constructing a fear hierarchy, ranking situations from least to most anxiety-provoking. Clients then learn relaxation skills, such as deep breathing or progressive muscle relaxation.
Exposure commences with the least anxiety-inducing item on the hierarchy, while the client actively employs their relaxation techniques. Progression occurs only when the client can experience the stimulus with minimal anxiety.
This gradual ascent continues, systematically desensitizing the individual to increasingly challenging situations, ultimately reducing avoidance behaviors and fostering a sense of control.
Flooding Techniques
Flooding, a more intensive exposure therapy method, involves confronting the feared stimulus directly and intensely for a prolonged period. Unlike systematic desensitization’s gradual approach, flooding aims for rapid habituation by overwhelming the anxiety response.
This technique requires careful consideration and is typically reserved for specific cases where a gradual approach proves ineffective or impractical. It’s crucial to ensure the client understands the process and provides informed consent.
During flooding, the client remains in the anxiety-provoking situation without engaging in avoidance behaviors, allowing their anxiety to peak and subsequently diminish as their physiological arousal subsides.
While potentially effective, flooding carries a higher risk of client distress and requires skilled clinical management to prevent adverse reactions. Proper preparation and support are paramount for successful implementation.

Specific Applications of CBT
CBT effectively treats diverse conditions like anxiety, depression, and addiction, showcasing its broad applicability and adaptability to individual client needs.
Trauma-Focused CBT (TF-CBT) aids children processing trauma, while Cognitive Processing Therapy (CPT) targets PTSD, reshaping traumatic event perceptions.

CBT for Anxiety Disorders
Cognitive Behavioral Therapy stands as a cornerstone in treating various anxiety disorders, offering a structured and effective approach to managing distressing symptoms. CBT helps individuals identify and challenge the negative thought patterns that fuel anxiety, replacing them with more balanced and realistic perspectives.
Techniques like cognitive restructuring are pivotal, enabling patients to reframe anxious thoughts and reduce their intensity. Simultaneously, behavioral techniques, such as exposure therapy, gradually introduce individuals to feared situations or objects in a safe and controlled environment.
Systematic desensitization, a component of exposure therapy, pairs relaxation techniques with gradual exposure, diminishing anxiety responses over time. CBT empowers individuals with coping mechanisms to navigate anxiety-provoking situations, fostering a sense of control and reducing avoidance behaviors. Ultimately, CBT aims to equip patients with the skills to manage anxiety independently and improve their overall quality of life.
CBT for Depression
Cognitive Behavioral Therapy proves highly effective in addressing depression, focusing on the interconnectedness of thoughts, feelings, and behaviors. A central tenet involves identifying and modifying negative thought patterns that contribute to depressive symptoms, such as feelings of hopelessness and worthlessness.
Behavioral activation, a key CBT technique, encourages individuals to re-engage in activities that once brought them pleasure, combating the withdrawal and inactivity often associated with depression. This proactive approach helps rebuild positive reinforcement and improve mood.
Cognitive restructuring challenges irrational beliefs and promotes more balanced thinking, fostering a more optimistic outlook. CBT equips individuals with practical coping skills to manage depressive symptoms, prevent relapse, and enhance their overall well-being, ultimately leading to a more fulfilling life.
Trauma-Focused CBT (TF-CBT)
Trauma-Focused Cognitive Behavioral Therapy (TF-CBT) is a specialized treatment approach designed for children and adolescents who have experienced traumatic events. It emphasizes a safe and supportive therapeutic environment where young individuals can process their experiences and develop coping mechanisms.
TF-CBT integrates several components, including psychoeducation about trauma, relaxation techniques, cognitive processing of traumatic memories, and development of coping skills. A crucial element involves the supportive involvement of caregivers, fostering a sense of safety and security.
The therapy aims to reduce trauma-related symptoms, such as anxiety, depression, and behavioral problems, while also enhancing the child’s self-esteem and overall functioning. It empowers young people to regain control and build resilience in the aftermath of trauma, promoting long-term healing and well-being.
Cognitive Processing Therapy (CPT) for PTSD
Cognitive Processing Therapy (CPT) stands as an evidence-based psychotherapy specifically tailored for individuals grappling with Post-Traumatic Stress Disorder (PTSD). Its core objective revolves around assisting patients in effectively processing traumatic events, challenging and ultimately modifying maladaptive beliefs stemming from those experiences.
CPT operates on the premise that PTSD often arises from difficulties in processing the cognitive and emotional aftermath of trauma. The therapy guides individuals to identify and evaluate “stuck points” – beliefs about themselves, others, and the world that contribute to distress.
Through a structured approach involving written accounts of the trauma and cognitive restructuring exercises, CPT aims to facilitate a more balanced and adaptive understanding of the event, reducing symptoms and improving overall functioning. It empowers individuals to reclaim their narrative and move forward.
CBT for Addiction
Cognitive Behavioral Therapy (CBT) proves remarkably effective in addressing addiction, functioning by identifying and modifying the thought patterns, emotional responses, and behavioral habits that perpetuate substance use or compulsive behaviors. It’s a highly adaptable approach, tailored to specific addiction types.
CBT helps individuals recognize triggers – internal cues like stress or cravings, and external cues like people or places – that prompt addictive behaviors. Therapists then collaborate with clients to develop coping strategies to manage these triggers without resorting to substance use or harmful actions.
Key techniques include craving management, relapse prevention planning, and addressing co-occurring mental health conditions. CBT empowers individuals to build self-control, develop healthier coping mechanisms, and ultimately achieve sustained recovery, fostering a life free from addiction’s grip.

CBT and Specific Populations

CBT adapts effectively for diverse groups, including children, adolescents, and individuals with conditions like misophonia, offering tailored interventions for unique needs.
CBT for Children and Adolescents
Cognitive Behavioral Therapy demonstrates remarkable efficacy when tailored for younger individuals, addressing a spectrum of challenges like anxiety, depression, and behavioral issues.
Adaptations are crucial; techniques are often presented through play, art, and age-appropriate language, fostering engagement and understanding in children and adolescents.

Parental involvement frequently forms a cornerstone of treatment, equipping parents with strategies to support their child’s progress and reinforce learned skills at home.
TF-CBT (Trauma-Focused Cognitive Behavioral Therapy) is a specialized approach for children who have experienced trauma, providing a safe and structured environment to process difficult experiences.
Focusing on identifying and modifying negative thought patterns, CBT empowers young people to develop healthier coping mechanisms and build resilience in the face of adversity.
Collaborative efforts between the therapist, child, and family are essential for successful outcomes, creating a supportive network for lasting positive change and improved wellbeing.
CBT for Individuals with Misophonia
Cognitive Behavioral Therapy offers a promising avenue for managing the intense distress experienced by individuals with misophonia, a condition characterized by heightened sensitivity to specific sounds.
Treatment typically focuses on identifying and challenging the negative thought patterns and emotional reactions triggered by these sounds, reducing their impact on daily life.
Exposure therapy, a core CBT technique, can be carefully implemented to gradually desensitize individuals to trigger sounds, lessening the associated anxiety and aversion.
Cognitive restructuring helps patients reframe their perceptions of trigger sounds, diminishing their perceived threat and promoting more adaptive responses.
Relaxation techniques, such as deep breathing and mindfulness, are often incorporated to manage the physiological arousal associated with misophonic reactions.
Support and education are vital components, empowering individuals and their families to understand misophonia and develop effective coping strategies for improved wellbeing.
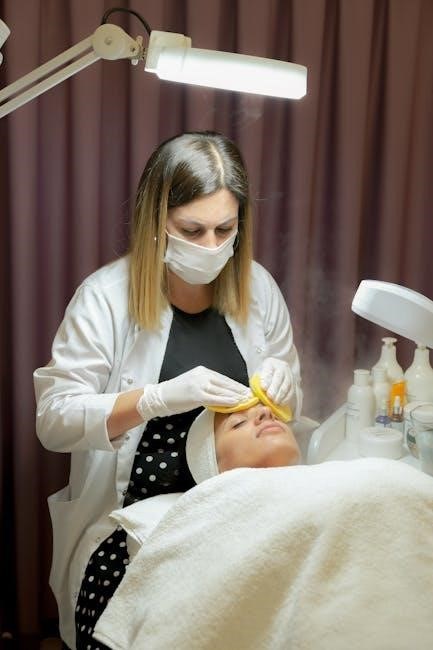
The Future of CBT
CBT is evolving through integration with other therapies and leveraging technological advancements, expanding access and personalization for enhanced mental healthcare outcomes.
Integration with Other Therapies
CBT’s remarkable flexibility allows for seamless integration with diverse therapeutic modalities, enhancing treatment efficacy and addressing complex patient needs comprehensively.
Combining CBT with psychodynamic therapy can explore underlying emotional patterns while equipping patients with practical coping skills, fostering deeper self-awareness.
Mindfulness-based approaches, when paired with CBT, cultivate present-moment awareness, reducing reactivity to negative thoughts and promoting emotional regulation.
Acceptance and Commitment Therapy (ACT) complements CBT by emphasizing values-driven action, even amidst difficult emotions, fostering psychological flexibility.
Dialectical Behavior Therapy (DBT), initially developed for Borderline Personality Disorder, integrates CBT with mindfulness and emotional regulation skills.
Neurofeedback, alongside CBT, offers potential for directly influencing brain activity associated with anxiety and depression, augmenting therapeutic gains.
This integrative approach acknowledges the multifaceted nature of mental health, tailoring interventions to individual circumstances for optimal outcomes.
Technological Advancements in CBT
The digital revolution is profoundly reshaping CBT delivery, expanding access and enhancing treatment personalization through innovative technological tools.
Mobile applications deliver CBT exercises, thought diaries, and psychoeducation directly to patients’ smartphones, promoting self-management and consistent practice.
Online CBT platforms offer remote therapy sessions, overcoming geographical barriers and increasing convenience for individuals with busy schedules.
Virtual reality (VR) exposure therapy creates immersive simulations of feared situations, facilitating safe and controlled exposure for anxiety disorders.
Artificial intelligence (AI) powered chatbots provide automated CBT support, offering personalized feedback and guidance between therapy sessions.
Wearable sensors monitor physiological data, such as heart rate variability, providing objective insights into stress levels and emotional responses.
These advancements promise to democratize mental healthcare, making evidence-based CBT interventions more accessible and affordable globally.